Love working with patients, hate writing therapy progress notes? You’re not alone. Most health practitioners love helping their patients but dread the paperwork of private practice.
Unfortunately, there’s no getting around creating these standard medical records. Therapy progress notes are important for monitoring the efficacy of treatments and communicating patient information. They are also essential for the filing of health insurance reimbursement claims.
“Every keystroke saved, is time saved, which means I can do my job longer and see more children.” — Dr. Melanie Hsu
While you can’t do away with therapy progress notes completely, you can use TextExpander to make completing them easier.
The fastest way to write therapy notes
TextExpander is a shorthand typing tool that lets you summon up words, phrases, and templates with just a couple of keystrokes.
(Read this article: What is TextExpander?)
Using TextExpander, you can create templates for therapy progress notes and make them appear on any page or platform with minimum typing.
TextExpander has several customization features, so you can create customizable templates. For example, you can add form fields, checkboxes, and dropdown lists to make them even easier to fill out.
TextExpander is also a wonderful tool for storing repetitive codes, terms, and phrases. You can create a library of standard medical terms, phrases, and descriptors on TextExpander to add them to documents without having to fully type them.
Dr. Jeremy Sharp, aka The Testing Psychologist, uses TextExpander to insert diagnostic codes, write results sections, populate recommendations, and sign reports. He created a series of helpful videos to illustrate how he does this — we recommend checking them out!
Write therapy progress notes faster
Here are some tips for writing therapy progress notes more quickly.

Use templates for therapy progress notes
SOAP, BIP, DAP, PIRP, BIRP. No matter what type of therapy progress note you use, there’s a template for it.
And that’s a good thing because templates save you time and eliminate the need for creating records from scratch.
Electronic health record (EHR) software programs usually have options. However, if you do not have EHR software, you can search for templates online, download them, and adapt them to your needs.
In fact, designing your own template might be the best option, because it gives you the flexibility to create the perfect note for your unique needs.
Use a ready-made template or design your own; just don’t waste time typing therapy progress notes from scratch.
Use checkboxes and dropdown lists
When creating your own progress note template, or adapting an existing one, be sure to add checkboxes, dropdown menus, and similar features whenever possible.
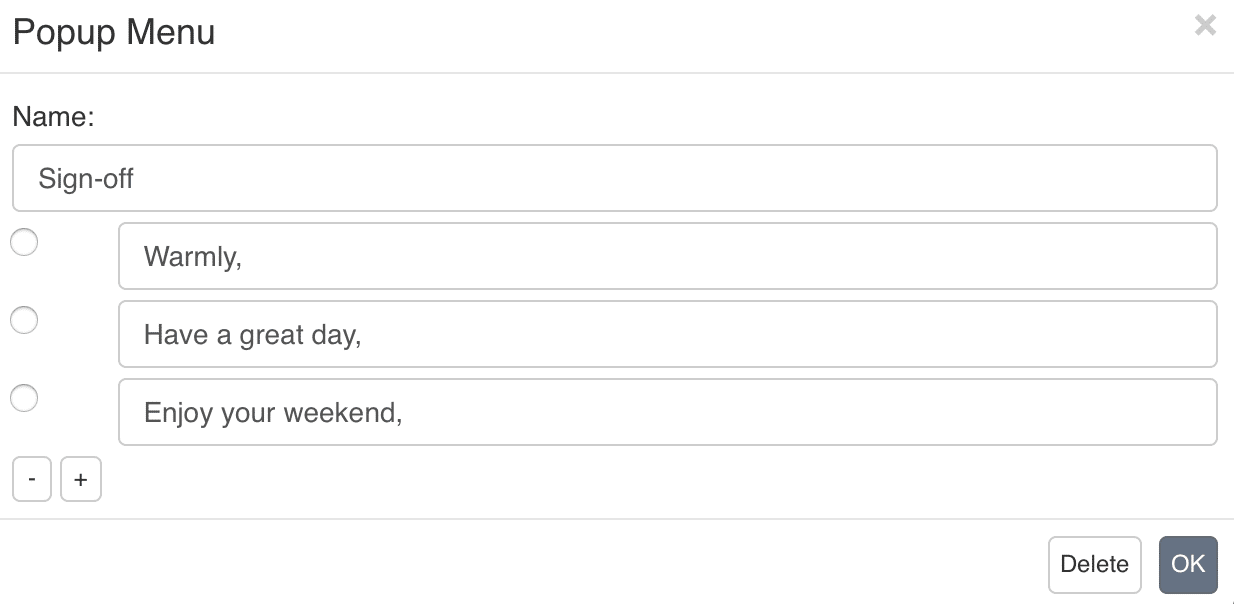
Having lists of items to select, as opposed to just fill-in-the-blanks form fields, saves you time since it reduces the amount of searching and typing that you need to do.
Lists and menus also have the advantage of preventing spelling errors and freeing you from having to rely on memory to add specific, hard-to-remember information.
Save standard terms, phrases, and descriptors
Repetitive language is standard in therapy progress notes. For example, “The patient presents symptoms of anxiety and depression” is a phrase you might write in the therapy progress notes of all patients suffering from anxiety and depression.
Instead of typing these standard terms, phrases, and descriptors from scratch each time, you can type them only once and save them so that you can easily access and use them in the future.
The idea is to create a library of standard phrasing and vocabulary — including intervention words, patient presentation descriptions, themes of sessions, treatment approaches, diagnostic codes, and more — so you can add them to your therapy progress notes without having to fully type them.
If you do not have software that provides this already, you can create your own lists of frequently-used terms and phrases. Some of these lists are available online — this list of commonly used intervention words for mental health progress notes is an example.
“Progress notes planner”-style books such as this one also provide a comprehensive catalog of health-related terms and descriptions for different types of practices.
Related questions
How long should it take to write therapy notes?
It all depends on how you take your notes, how thorough you need to be, and whether or not you use tools to help you type faster. While some therapists claim to spend between two to five minutes on each progress therapy note, most agree that at least fifteen minutes are necessary to reflect upon a 45-minute session.
How do you catch up on therapy notes?
“Start writing your current notes each day and come up with a system for clearing away the backlog. When this happened to me, I wrote a list of which clients had unfinished notes and tackled a few clients each day until I was caught up,” April Snow, LMFT from SensitiveTherapist.com, wrote.
Even if you can’t remember anything from the session, make a note anyway. “It’s best to have a note in the file, even if it’s sketchy. Include the basic information needed for billing: date, the start and stop time, the location of the session, the CPT code, and a general description, like ‘continued to work on progress toward treatment goals.’ This is better than nothing. At the end of the note, include the date of the next session to indicate continuity of care, as well as the date the note was written,” Beth Rontal wrote on the blog Documentation Wizard.
How do you write a good mental health progress note?
A good mental health progress note is clear, concise, and professional in tone. One of the easiest ways to write a good mental health progress note is to use the SOAP (Subjective, Objective, Assessment, and Plan) format.
What should be included in a therapy note?
As per the SOAP format, a therapy note should have four components: Subjective, Objective, Assessment, and Plan.
- The Subjective component includes the Chief Complaint (a quote from the patient about what brought them to therapy); the History of Present Illness (the patient’s condition from the initial symptom to the present state); the History (pertinent medical history); and a review of symptoms.
- The Objective component includes information that the therapist or healthcare provider can observe, such as the physical presentation or psychological status.
- The Assessment component is a description of the main symptoms, typically accompanied by a diagnosis (or list of possible diagnoses) and/or possible causes.
- The Plan component is a description of what the health provider will do to treat the patient.
Try TextExpander free for 30 days
TextExpander saves therapists and other health care professionals hours each month by eliminating the need to type repetitive words, codes, and phrases fully.
Incorporating TextExpander into your workflow will not only help you complete therapy progress notes faster, but will save you time that you can use to focus on work that really matters to you.

